Nationally, physicians are encountering more patients reporting symptoms of major depressive disorder, with 30.9% of this patient population presenting with a treatment-resistant form of the condition, according to research published in the Journal of Clinical Psychiatry.
Patients with treatment-resistant depression may benefit from one or more of the treatment modalities offered through the Institute for Advanced Diagnostics and Therapeutics at Sheppard Pratt, which has been established to provide expert clinical care for depression and certain other psychiatric illnesses using long-standing and newly developing treatments, including transcranial magnetic stimulation (TMS) and electroconvulsive therapy (ECT).
Transcranial magnetic stimulation (TMS) is a modality that directs magnetic pulses at specific areas of the brain to generate small electrical currents. Approved by the U.S. Food and Drug Administration (FDA) in 2008 for treatment-resistant depression, TMS treatments are provided daily (5 days a week) for up to six weeks, depending on patient needs. No anesthesia is required, and treatments are well tolerated. The most frequently reported side effect is a temporary headache during the first week of treatment. Patients can still work, attend school, and maintain a regular schedule while receiving treatment. Sheppard Pratt has been at the forefront of clinical trials for TMS and has deep expertise in this treatment modality.
Patricia Carlson, MD, service chief of Sheppard Pratt’s TMS program, would like TMS to become a more accessible option to treat depression. “Too many people struggle with treatment-resistant depression when safe and effective treatment options are available,” Dr. Carlson says.
Patients receiving TMS generally experience a gradual lifting of their mood a few weeks into treatment. “Both in my years of administering TMS and in several peer-reviewed studies, we have observed that the majority of patients who had a good response are still seeing benefits six months after treatment without having to reinitiate,” Dr. Carlson says. Some patients can benefit from ongoing or intermittent “booster” treatments to keep moods optimized.
-
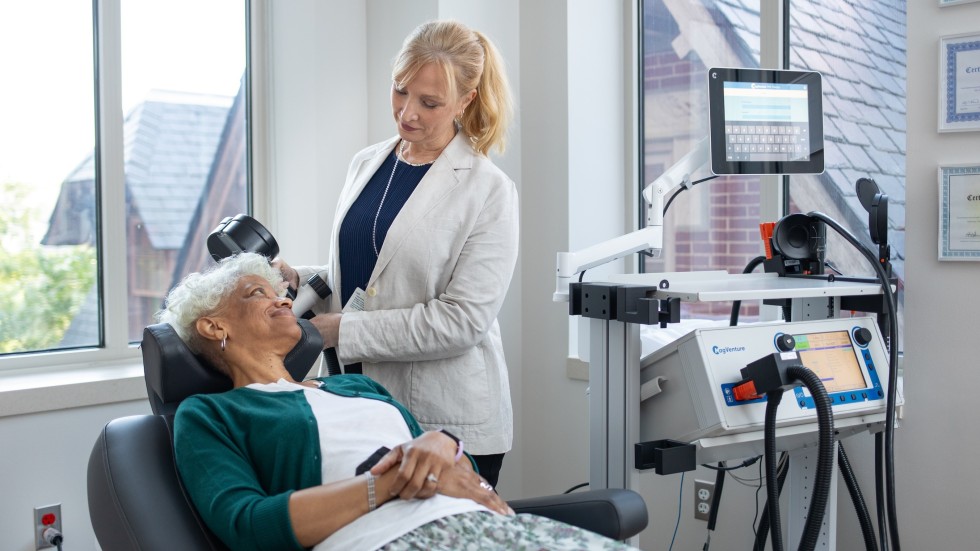
Transcranial magnetic stimulation is a nonsystemic, highly effective treatment option for difficult-to-treat depression.
-

Monica Rettenmier, MD, conducts electroconvulsive therapy sessions for patients once they are safely under anesthesia.
ECT is another neuromodulation treatment available at Sheppard Pratt. Once known as electroshock therapy, this therapeutic treatment option has been in use since the 1930s. However, ECT has undergone a significant change in terms of delivery, safety, and overall tolerability. It has been used successfully and increasingly in the United States since the 1990s. Patients are treated under anesthesia in a series of sessions every other day for several weeks. ECT has proven benefits for patients with unipolar and bipolar depression, severe postpartum depression, suicidal ideation, catatonia, psychosis, and other conditions.
Monica Rettenmier, MD, child and adolescent psychiatrist and ECT service chief for Sheppard Pratt, explains that ECT is an option for patients when medications and other interventions have failed to improve symptoms. ECT is also an option when medication can’t be given or isn’t well tolerated, such as during pregnancy or for older adults. Other patients may opt to try ECT if they are averse to taking medication.
“Sheppard Pratt offers a Provider Help Line for physicians who want to review treatment options for their patients. We can have a 20-minute discussion with them to run through the case and discuss all of the options,” Dr. Rettenmier says.
She explains that patients who undergo ECT may experience a lessening of their depression within the first few weeks of treatment. The treatment is well tolerated, although some patients experience brain fog. After ECT, patients are encouraged to maintain their medication regimen because without continued stabilization, patients are far more likely to experience a re-emergence of their acute psychiatric illness and need additional treatments.
“For some patients, though, even with continued medications, therapy, and lifestyle changes, their depression resurfaces after ECT is discontinued,” says Dr. Rettenmier. “This may occur within a few weeks, months, or maybe years later. For these individuals, further treatment in a maintenance schedule may help to maintain their mood stability.
“We have a small to moderate cohort of maintenance patients who have been with us for 15 or 20 years,” she continues. “Depending on the needs of the patient, treatment sessions are spaced four to 12 weeks apart and are part of what keeps them safe, stable, out of the hospital, and not suicidal.”
With either treatment, Sheppard Pratt clinicians work closely with referring physicians to ensure each patient’s care is appropriate and tailored to their specific needs. 
The Institute for Advanced Diagnostics and Therapeutics
The institute brings expert clinical care of difficult-to-treat illnesses together with a center of research developing brand new treatment modalities
Featured Experts
-

Trish Carlson, MD
Service Chief, TMSSpecialties:Adult Psychiatry, Anxiety Disorders, Dialectical Behavior Therapy (DBT), Eating Disorders, LGBTQ+ Mental Health Issues, Mood Disorders, Transcranial Magnetic Stimulation (TMS), Transference-focused Psychotherapy, Treatment-resistant Depression